Arrhythmia: Understanding the Types, Causes, Symptoms, and Treatment

Introduction An arrhythmia is any heartbeat that is too fast, too slow, or irregular. It happens when the electrical impulses that make the heart beat properly do not work right. Most people have experiences of mild arrhythmia that does no harm at all; very few live with some graver, life-threatening version of the disorder. In this article, we will look into the various types, causes, symptoms, treatments, and complications of arrhythmia, giving a well-rounded understanding of the heart condition and how to seek adequate treatment. What Arrhythmia Is? Any abnormal rhythm of the heart is referred to as arrhythmia. The heart relies on electricity to function, and when something goes wrong in these electrical signals, an irregular heartbeat occurs. The heartbeat is supposed to be regular; however, in arrhythmia, the heartbeat could become too fast-sometimes called tachycardia-, too slow, bradycardia, or irregular. It can be harmless, or it could risk your heart health, depending upon the kind and severity. Types of Arrhythmia There are so many arrhythmias, and they differ in severity and the degree to which they affect how the blood is pumped into circulation. Most common are the following types of arrhythmias: Atrial Fibrillation (AFib): It is one of the most common arrhythmias occurring when the atria-upper chambers of the heart-anyhow beat irregularly and fast. AFib creates a situation of risk for stroke and, if untreated, may result in heart failure. Ventricular Tachycardia (VT): This is a condition where the ventricles-the lower chambers of the heart-are too fast in beating. It could be lethal and may lead to a reduction in the heart’s ability to pump blood. Bradycardia: A heart rate slower than normal and, generally, under 60 beats per minute. It may be harmless in some respect, but it can lead to dizziness, fainting episodes, or heart failure if extreme. Supraventricular Tachycardia (SVT): This is a type of fast heartbeat starting somewhere above the ventricles. Usually not a cause for concern, SVT can cause palpitations, dizziness, or even discomfort in the chest. Premature Ventricular Contractions (PVCs): These are extra heartbeats that originate from the ventricles. While not really harmful in most cases, PVCs are actually considered a nuisance by many who experience them. Ventricular Fibrillation (VFib): It is a cardiac emergency in which the ventricles quiver rather than resulting in blood pumping. Within minutes without treatment, VFib equals sudden cardiac arrest. You can read also:- Blood Clot in Brain: Types, Reasons & Treatment Causes of Arrhythmia There are different causes of arrhythmia, ranging from lifestyle and health-related factors to something more grave, such as heart conditions. Some very usual causes are: Coronary Artery Disease (can be): The arteries may be blocked or perhaps narrowed; in such cases, the heart gets distanced from receiving an arrhythmia due to restricted blood flow. Heart Attack: Heart muscle that has been damaged during or after the heart attack can disrupt the electrical signals responsible for regulating heartbeats. High Blood Pressure: High blood pressure within chronicle time enlarges the heart, thus leading to arrhythmias. Congenital heart defects: Sometimes people are born with defects in the heart that influence the rhythm of the heart. Electrolyte Imbalances: An imbalance in potassium, sodium, or other electrolytes can interfere with the heart’s electrical impulses. Thyroid Disorders: The arrhythmias associated can be either hyperthyroidism or hypothyroidism. Stimulants: Caffeine, alcohol, some medications, and maybe even some recreational drugs can probably induce arrhythmias. Symptoms of Arrhythmia Sometimes there are no symptoms of an arrhythmia, whereas, if symptoms do occur, they differ according to the type and severity of the condition. Some prominent types are as follows: Palpitations: The heart is felt to be fluttering, pounding, or racing. Dizziness or Lightheadedness: Because the heart is unable to pump enough blood to the brain. Shortness of Breath: Difficulty in breathing on exertion or lying flat. Chest Pain or Discomfort: It can vary from mild pressure to agonizing pain. Fatigue: Being unusually tired or weak because of poor circulation. Syncope or Near-Syncope: Insufficient blood supply to the brain. How Are Arrhythmias Treated? Treatment for arrhythmias depends on the type and severity of the condition and the general health of the patient. Typical treatment modes are as follows: Drugs: Antiarrhythmic drugs help with the control of heart rhythm. Blood thinners may be prescribed in cases where there is a high risk of stroke, especially in people with AFib. Cardioversion: In this intervention, the patient is given a controlled shock to convert an abnormal rhythm. It is generally employed for patients with atrial fibrillation or other forms of tachyarrhythmias. Catheter Ablation: This basically employs a catheter that is passed through the blood vessels to the heart, which is destroyed in some way, causing abnormal electric signals. Pacemaker: The pacemaker is a small battery-operated device implanted subcutaneously to pace a slow heart rate by sending electrical impulses to the heart to maintain normal rhythm. Implantable Cardioverter-Defibrillator (ICD): An ICD is an implantable device in the chest used for the detection of the heart rhythm and the delivery of shocks if it is faced with the detection of life-threatening arrhythmias like ventricular fibrillation (VFib). Lifestyle Changes: Or mild arrhythmias in people, lifestyle modifications may be adequate. Included in this category would be reducing caffeine and alcohol intake, stress management, regular exercise, and avoiding stimulants. Surgical Intervention: Sometimes surgery is just what is needed to correct structural abnormalities causing arrhythmias. You can read also:- Blood Sugar Level Chart: A Simple Guide to Normal Ranges Complications of Untreated Arrhythmia Untreated arrhythmia may cause a number of grave health problems, including:Stroke: Some arrhythmias, like atrial fibrillation, make you more apt to develop clots obstructed in the brain to cause stroke. Heart Failure: Arrhythmias, when chronic, have a weakening effect upon the heart so that its capacity to pump blood is altered.Sudden Cardiac Arrest: In more serious forms, arrhythmias such as ventricular fibrillation render the heart to sudden standstill, resulting in death if not given immediate rescue. Arrhythmia Prevention Some of the arrhythmia risk factors such as genetics cannot
हार्ट पेसमेकर कब लगाना और क्यों ज़रूरी है? प्रक्रिया और देखभाल के आसान टिप्स
आजकल की इस भाग दौड़ भरी जिंदगी में देखा जाए तो गलत खानपान और गलत रहन सहन की वजह से दिल की समस्याएं बहुत ही आम हो गई है, इसी वजह से हार्ट अटैक के केस बहुत ज्यादा बढ़ रहे हैं । तब आज हार्ट अटैक आता है, जब हम अस्पताल में जाते हैं तो आपने देखा होगा डॉक्टर कहते हैं कि इसको तो पेसमेकर लगवाना पड़ेगा या इसकी पेसमेकर सर्जरी होगी। बहुत सारे लोगों के मन में यह सवाल रहता है कि ” पेसमेकर (heart pacemaker) होता क्या है, पेसमेकर सर्जरी होती क्या है और यह कैसे की जाती है आज हम इसी बारे में ब्लॉग के माध्यम से विस्तार से जानकारी देंगे। पेसमेकर क्या है और यह कैसे काम करता है? (What is a pacemaker and how does it work?) सबसे पहला सवाल होता है कि पेशमकर होता क्या है(Pacemaker Kya Hota hai), तो बता दे आपको की पेसमेकर एक छोटा सा एवं इलेक्ट्रॉनिक डिवाइस होता है, जिसे डॉक्टर त्वचा के नीचे छाती के पास सर्जरी की सहायता से इंप्लांट करते हैं। आपको जानकारी आश्चर्य होगा कि इसी उपकरण की मदद से हार्ट सर्जन अपने चेंबर में बैठकर आपका हृदय की गतिविधि को आसानी से ट्रैक भी कर सकते हैं और नियंत्रित भी कर सकते हैं। दूसरा मन में सवाल रहते हैं कि यह काम क्या करता है, तो आपको बता दे कि यह उपकरण आपका हृदय की धड़कन को सामान्य बनाए रखने में हेल्प कर सकता है। पेसमेकर आपके दिल की धड़कन की ले को भी नोट करता है और समय-समय पर इसकी रीडिंग को डॉक्टर को भेजता रहता है अगर आपकी धड़कन धीमी हो जाती है या अनियमित हो जाती है, तो पेसमेकर उसे ठीक करने का काम करता है। पेसमेकर कब और क्यों लगाया जाता है? (When and why is a pacemaker implanted?) पेसमेकर (heart pacemaker लगाने की ज़रूरत मरीज तब पड़ती है जब हृदय की प्राकृतिक पेसमेकिंग प्रणाली (जिसे साइनस नोड कहते हैं) ठीक से काम नहीं करती। इसके कुछ मुख्य कारण हैं: धीमी धड़कन (ब्रैडीकार्डिया): अगर हृदय की धड़कन 60 धड़कन प्रति मिनट कम हो जाती है, तो थकान, चक्कर आना या बेहोशी जैसी समस्याएँ हो सकती हैं। ऐसी स्थिति में, “पेसमेकर कब लगाया जाता है” का जवाब धड़कन को तेज़ करना है। हार्ट ब्लॉक: यह तब होता है जब हृदय के ऊपरी और निचले हिस्सों के बीच सिग्नल ब्लॉक हो जाते हैं। डॉक्टर एट्रियोवेंट्रीकुलर ब्लॉक या साइनस नोड डिसफंक्शन जैसी स्थितियों में पेसमेकर लगाने की सलाह देते हैं। अन्य हृदय रोग: इसे हृदय गति रुकने, अलिंद विकम्पन या पहले हुए हृदयाघात के बाद भी लगाया जा सकता है। अगर आप “पेसमेकर क्यों लगाया जाता है” खोज रहे हैं, तो याद रखें कि यह एक जीवन रक्षक उपकरण है जो हृदय को नियमित धड़कन देने में मदद करता है। उम्र और अन्य कारक: यह बुजुर्गों में ज़्यादा आम है, लेकिन युवाओं में दवाओं के दुष्प्रभाव या जन्मजात समस्याएं भी पैदा कर सकता है। डॉक्टर ईसीजी, होल्टर मॉनिटरिंग या अन्य जाँचों के बाद ही कोई निर्णय लेते हैं। अगर आपको चक्कर आ रहे हों या साँस फूल रही हो, तो तुरंत डॉक्टर से संपर्क करें – यह पेसमेकर की ज़रूरत का संकेत हो सकता है। You can read also:- Blood Clot in Brain: Types, Reasons & Treatment पेसमेकर लगाने की प्रक्रिया (Pacemaker implantation procedure): चरण दर चरण “पेसमेकर सर्जरी” (heart pacemaker Surgery) सुनकर डर लगता है, लेकिन यह एक आसान प्रक्रिया है जो लोकल एनेस्थीसिया के तहत होती है। इसमें लगभग 1-2 घंटे लगते हैं। यहाँ देखें कैसे: तैयारी: सर्जरी से पहले रक्त परीक्षण, ईसीजी और एक्स-रे होते हैं। आपको उपवास रखना पड़ सकता है। प्रक्रिया: डॉक्टर छाती के ऊपरी हिस्से में एक छोटा सा चीरा लगाते हैं। पेसमेकर त्वचा के नीचे पेसमेकर लगाते हैं और नसों के माध्यम से हृदय तक तार (लीड्स) पहुँचाते हैं। सभी जाँचें फ्लोरोस्कोपी (एक प्रकार का लाइव एक्स-रे) से की जाती हैं। समापन: चीरा बंद करें और पट्टी बाँधें। अधिकांश मरीज़ उसी दिन या अगले दिन घर जा सकते हैं। यह प्रक्रिया सुरक्षित है, लेकिन इसमें संक्रमण या रक्तस्राव जैसे जोखिम हो सकते हैं। इसलिए, हमेशा अनुभवी हृदय रोग विशेषज्ञों से सलाह लें। You Can Read also:- डॉक्टर के पर्चे का मतलब: दवा के पर्चे में कोड और डॉक्टर की लिखावट को समझें पेसमेकर के बाद देखभाल के सुझाव: स्वस्थ रहने के आसान तरीके पेसमेकर के बाद जीवन सामान्य हो जाता है, लेकिन कुछ सावधानियां ज़रूरी हैं। “पेसमेकर के बाद देखभाल” के लिए यहाँ कुछ व्यावहारिक सुझाव दिए गए हैं: आराम और रिकवरी: सर्जरी के 1-2 हफ़्ते बाद तक भारी काम न करें। चीरे वाली जगह को साफ़ रखें और डॉक्टर द्वारा दी गई दवाएँ समय पर लें। आहार और व्यायाम: स्वस्थ आहार लें – फल, सब्ज़ियाँ, कम नमक और वसा। हल्का टहलना शुरू करें, लेकिन डॉक्टर की सलाह से। धूम्रपान और शराब से दूर रहें। नियमित जाँच: हर 3-6 महीने में पेसमेकर की जाँच करवाएँ। अगर बैटरी 5-10 साल तक चलती है, तो समय पर बदलवा लें। सावधानियाँ: तेज़ चुंबकीय क्षेत्र (जैसे एमआरआई मशीन) से दूर रहें। हवाई अड्डे की सुरक्षा में अपना पेसमेकर कार्ड दिखाएँ। मोबाइल फ़ोन को पेसमेकर वाली जगह से दूर रखें। आपातकालीन सुझाव: अगर दिल की धड़कन असामान्य लगे या दर्द हो, तो तुरंत डॉक्टर से मिलें। याद रखें, पेसमेकर से ज़िंदगी बेहतर है – कई लोग सालों तक सक्रिय रहते हैं। निष्कर्ष हृदय पेसमेकर (heart pacemaker) एक चमत्कारी आविष्कार है जो लाखों लोगों की जान बचाता है। अगर आप “हृदय पेसमेकर जानकारी” या “पेसमेकर उपचार” खोज रहे हैं, तो उम्मीद है कि यह ब्लॉग आपके लिए उपयोगी होगा। लेकिन ध्यान दें, यह सामान्य जानकारी है – वास्तविक सलाह के लिए डॉक्टर से बात करें। किसी भी हृदय संबंधी बीमारी के इलाज के लिए जयपुर के सर्वश्रेष्ठ अस्पताल Rungta Hospital में अपॉइंटमेंट बुक करें और सही इलाज पाएं। अक्सर पूछे जाने वाले प्रश्न पेसमेकर लगाने के बाद क्या खाना चाहिए? Ans. हार्ट पेसमेकर लगने के बाद मरीज को किसी विशेष आहार की ज्यादा जरूरत तो नहीं होती है, लेकिन एक हृदय को स्वस्थ रख सके ऐसा आहार लेने की सलाह डॉक्टर पेशेंट को देते हैं। इसमें फल, सब्जियां, होल ग्रेन्स और लीन
Anal Fissure: What It Is, Symptoms, Causes & Treatment
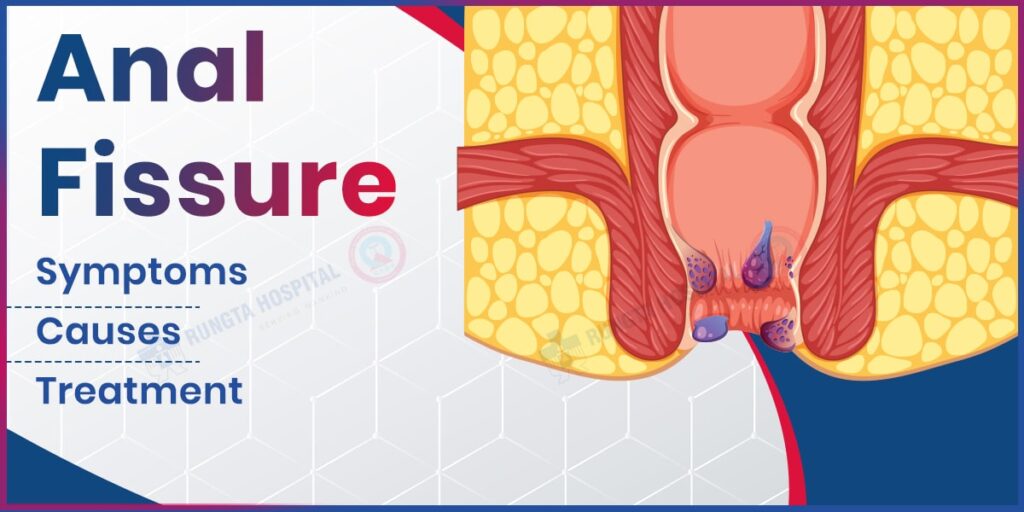
Introduction Understanding the meaning of fissure in medical terms enables a person to understand the fissure and its treatment better. However, it becomes an article of discomfort in an individual’s life when it is accompanied by pain along with bleeding after passing stool. Small tears, fissures in the anal canal, usually cause great pain during and following defecation. They stop a man from living a normal life. In this regard, people can understand the pain experienced by the common symptoms of fissure and their causes, which are examined in this write-up, along with fissure and its treatment. Recognizing the signs means that one can take action to ease the pain and help in the recovery process. What is an anal fissure? Anal fissures are a small tear or crack in the anus lining, more often than not caused by passing a stool that is either hard or large. An anal fissure can cause an individual to experience a combination of pain, bleeding, and discomfort while trying to defecate. While anal fissures can happen to anyone and are commonplace, practicing timely care and proper management will help in healing and preventing the fissures from happening again. Are anal fissures common? Certainly, fissures are benign or shallow cuts in the skin surrounding the anus, also known as the anal mucosa. Anal fissures strike people of any age, even infants, and are usually caused by straining during a bowel movement, lengthy bouts of constipation, or passing hard-shaped stools. Although a large number of fissures tend to heal spontaneously, chronic and recurrent fissures demand proper care and fissure treatment options timely to avoid further complications. You can read also:- Blood Clot in Brain: Types, Reasons & Treatment What are the symptoms of an anal fissure? One can identify the symptoms of anal fissure, and they can have severe discomfort while diagnosing the symptoms in the toilet, the first symptoms are: Pain during bowel movements: The duration has the symptom and is noticeable and this happens when you empty the bowel, you experience a burning, sharp or even a tearing sensation. It is commonly known as an anal … Bleeding: The anal leakage occurs when the anal lining has been torn. In this case the anal lining happens to be torn. Itching or Irritation: The anal opening has symptoms such as redness, inflamed skin which leads to continuous scratching. Visible Tear: In the more severe cases, a visible crack or tear appears on the skin around the anal opening. Spasms: The torn skin and muscle are exposed and act abnormally which means they are not functioning properly. In such cases, the healing process slows down and provides severe pain. Sitting Pain: After spending a lot of time sitting, anal pain or discomfort may worsen. How do I know if I have a hemorrhoid or an anal fissure? While both affect the anal area and may cause pain or bleeding, fissures and hemorrhoids differ in their own characteristics, which help in their identification. Pain Type and Timing: Anal fissures cause sharp, burning pain during and immediately after bowel movements, whereas hemorrhoids are associated with a persistent ache or throbbing, particularly when sitting down, and less sharp localized pain. Bleeding Type: An anal fissure will often present with bright red blood on the stool or toilet paper. Hemorrhoid bleeding may appear during bowel movement, usually noted as an obvious blood clot or as a “coat” of blood around the stool. Location: Most anal fissures occur on the posterior portion of the anal canal and most take place at the midline. Hemorrhoids can occur externally, around the anus, or internally – within the rectum – where they can develop as prolapsing swellings. Visible Signs: A fissure is open and often looks like a small lineal break in the skin around the anus. Swollen, dark blue lumps can point to an external hemorrhoid, and polyps may bulge outwards during periods when the anus is strained. Associated Symptoms: With hemorrhoids, there is often a “fullness” feeling, as well as tenderness, swelling, and a need to itch. The pain with anal fissures can be made worse by the spasming muscle cuts of the sphincter in the anus. What is the main cause of an anal fissure? The main cause of an anal fissure is trauma to the anal canal, usually due to hard, dry, or large stool. Overall, conditions that cause chronic constipation include: Frequent Straining while having a bowel movement: Pressure on the anal canal puts it in a position to be injured. Diarrhea: With multiple episodes of loose or watery stool, the anal tissue can become damaged or irritated. Child birth: Vaginal delivery can cause anal fissures due to increased pressure on the pelvis. Anal intercourse or trauma: Trauma to the anal area will likely result in a fissure. Other medical conditions: Trauma to the anal canal can be more easily caused by conditions such as Crohn’s or inflammatory bowel disease (IBD). You can read also:- Blood Sugar Level Chart: A Simple Guide to Normal Ranges How are anal fissures diagnosed? It is generally accepted that the assessment of medical history and symptoms are the first two steps in the course of an anal fissure diagnosis. The overall evaluations are aimed at determining: Medical History: The doctor will ask about the patient’s bowel movements, bleeding, and pain, and any relation to past anal, or gastrointestinal dysfunction. Physical Exam: In most cases, a fissure can be seen visually, especially when the fissure is in the midline in the anal area. Digital Rectal Exam: In some cases the doctor may require a brief anus examination with a single-gloved finger to determine whether deeper anal fissures are present, and if any further complications exist. Further Tests: If fissures are recurrent, chronic, or unusual, then the physician may recommend tests such as an anoscopy or sigmoidoscopy, or other tests to exclude diseases such as Crohn’s. What is the medical treatment for anal fissures? The goal of medical treatment for anal fissures is
Cancer Screening Tests: Know the Signs, Types & Guidelines
Introduction Early detection of cancer, even prior to the manifestation of any noticeable symptoms, is a crucial preventive step that enables advanced treatment and offers a higher chance of survival. Cancer screening is a testing method that is carried out to detect cancer at its earliest stage. Gaining knowledge of such testing procedures emails would enable an individual to actively participate in his or her health care. In this section, we intend to address the specific defining characteristics of cancer screening, the major indicators which trigger the screening, the different types of cancer screening, and the specific rules which dictate at what age or how often screening should be done. As previously mentioned, cancer prevention screening allows an individual to make thoughtful decisions on adopting a health regimen aimed at long term prevention and maintenance; hence this understanding is important. What is cancer screening? Cancer screening refers to a healthcare procedure aimed at testing individuals who are healthy or show no symptoms in order to identify cancer at its earliest stage before any symptoms present themselves. The primary objective of cancer screening is to detect any abnormal changes or early indications of cancer so that prompt treatment can be administered, the management can be successful, and the outcome can be favorable. What are the advantages of cancer screening? The advantages of any form of screening test include early identification of cancer and the prevention of cancer progression. Benefits of a screening test include. Early identification: With any disease, the sooner it is identified as a disease, the higher the chance of treatment. A screening test may identify cancer at an earlier stage when any treatment may be more successful and less invasive. Better survival rates: The sooner the cancer is identified using cancer screening tests, the higher the chance of successful treatment and survival rate. Prevention of Advanced Disease: Through certain screening tests, in the absence of detection, there is the possibility of precancerous changes, which means one can intervene prior to full-blown cancer. Better Treatment Options: When treatment is initiated early, there are greater options available, which means therapies are less aggressive and fewer complications are associated. Peace of Mind: Undetected cancer can be troubling; regular cancer screening tests help individuals who are at risk to be reassured and anxious free. Cost-Effective in the Long Term: The earlier cancer is detected, the less likely the patient is to undergo extensive treatment and hospitalization, and therefore there is less cost associated with healthcare. You can read also:- Blood Clot in Brain: Types, Reasons & Treatment Who should be screened for cancer? One can identify the symptoms of anal fissure, and they can have severe discomfort while diagnosing the symptoms in the toilet, the first symptoms are: Pain during bowel movements: The duration has the symptom and is noticeable and this happens when you empty the bowel, you experience a burning, sharp or even a tearing sensation. It is commonly known as an anal … Bleeding: The anal leakage occurs when the anal lining has been torn. In this case the anal lining happens to be torn. Itching or Irritation: The anal opening has symptoms such as redness, inflamed skin which leads to continuous scratching. Visible Tear: In the more severe cases, a visible crack or tear appears on the skin around the anal opening. Spasms: The torn skin and muscle are exposed and act abnormally which means they are not functioning properly. In such cases, the healing process slows down and provides severe pain. Sitting Pain: After spending a lot of time sitting, anal pain or discomfort may worsen. How do I know if I have a hemorrhoid or an anal fissure? Depending on one’s age, lifestyle, and family history, cancer screening is recommended for the efforts of early detection and prevention. Here are the primary groups that would need to undergo cancer screening tests: Adults in the Appropriate Age Groups: Most cancers have defined age groups for screening, like mammograms for women above 40 or colonoscopies for adults over 45. People with a Family History of Cancers: People whose close family members have contracted cancers are considered to have higher risk and may be required to undergo cancer screening tests earlier and more frequently. People with High-Risk Lifestyle Factors: Smoking, heavy drinking, bad dieting, and lack of exercise are considered high-risk in terms of developing cancer and thus demand a regular screening. People with a History of Previous Precancerous Conditions: Those who have undergone treatment for abnormal or precancerous tissues may be required to take follow-up cancer screening. People with Cancer-related Genetic Predispositions: People with cancer-associated inherited genetic mutations such as BRCA1 and BRCA2 require tailored screening protocols. What are cancer screening tests? The purpose of cancer screening tests is to find cancer or precancerous conditions early and cancer screening tests are of the following types: Mammography: This test is an X-ray of the breast, which is primarily aimed at finding any earliest signs of breast cancer, even before a lump can be detected by touch. Women over 40 should have regular mammograms, and those at greater risk should have them more often. Pap Smear (Cervical Screening): The procedure for a Pap smear collects cells from the cervix to detect either precancerous changes or cervical cancer. This test is usually indicated for women between the ages of 21 and 65, and can be performed together with HPV testing for more complete screening. Colonoscopy: A colonoscopy is an examination of the colon and rectum with a flexible tube with a camera to view the insides. This test is important in the detection of colon cancer and precancerous polyps and is usually recommended from the age of 45, or earlier for those who have a family history. Low-Dose CT Scan: This test is appropriate for lung cancer screening in adults aged 50 to 80, who have a heavy smoking history. It can find lung nodules of a small size which may show signs of lung cancer in its early
डॉक्टर के पर्चे का मतलब: दवा के पर्चे में कोड और डॉक्टर की लिखावट को समझें

ज़ब आपकी बॉडी मे कोई प्रॉब्लम आती है तो आप डॉक्टर के पास जाते हो और डॉक्टर आपकी बीमारी के इलाज के लिए एक पर्ची पर दवाई का नाम, खुराक (Dosage), लेने का समय जाँच और कुछ निर्देश लिखता है उसे हीं डॉक्टर का पर्चा कहा जाता है । लेकिन आम लोग मेडिकल क़ी भाषा क़ी समझ कम रखते है, तो डॉक्टर क़ी लिखावट समझ नहीं पाते है और उसमे लिखें कोड क़ी पहचान करना मुश्किल कार्य है। इस ब्लॉग में हम हिंदी और अंग्रेजी में डॉक्टर के पर्चे का मतलब, दवा के पर्चे पर इस्तेमाल होने वाले कोड और उनके मतलब और डॉक्टर की लिखावट को समझने के तरीके बताएंगे। डॉक्टर के पर्चे में क्या – क्या लिखा होता है? डॉक्टर का पर्चा जिसे एक ऐसा दस्तावेज कह सकते हैं जिसमें डॉक्टर मरीज को दवाइयाँ, उनकी मात्रा, लेने का समय और इलाज से संबंधित अन्य निर्देश देते हैं। यह चिकित्सक को दवा देने और मरीज को सही इलाज देने में मदद करता है। पर्चे में अक्सर निम्नलिखित विवरण शामिल होते हैं: मरीज का नाम और उम्र (Patient’s Name and Age), दवा का नाम (Medicine Name) दवा लेने का समय ((Dosage, जैसे 1 टैबलेट दिन में दो बार) इलाज की अवधि (Duration, जैसे 5 दिन तक) डॉक्टर की लिखावट क्यों पढ़ना मुश्किल है? डॉक्टरों को कम समय होने के कारण अक्सर उनकी लिखावट जल्दबाजी में लिखी जाती है। इसके अलावा, मेडिकल शब्द और कोड लैटिन भाषा (Latin Terms) या संक्षिप्त रूपों में लिखे जाते हैं, जो आम लोगों के लिए समझना मुश्किल होता है। आप भी पर्चे को आसानी से समझ सकते हैं अगर आप कुछ आम कोड और उनके मतलब जान जायेंगे। दवा के पर्चे में क्या कोड लिखे होते हैं? पर्चे में दवा लेने के तरीके, समय, और अन्य निर्देश छोटे-छोटे संक्षेपों (Abbreviations) से दर्शाए गए हैं। ये कोड लैटिन भाषा से लिए गए हैं, जो विश्व भर में मेडिकल क्षेत्र में उपयोग की जाती है। नीचे चार दर्जन सामान्य कोड और उनके हिंदी और अंग्रेजी अर्थ दिखाए गए हैं। 20 आम मेडिकल कोड और उनके अर्थ (40 Common Medical Codes and Their Meanings) कोड हिंदी अर्थ अंग्रेजी अर्थ OD दिन में एक बार Once a Day BD दिन में दो बार Twice a Day TDS दिन में तीन बार Three Times a Day QID दिन में चार बार Four Times a Day HS रात को सोते समय At Bedtime SOS जरूरत पड़ने पर As Needed PO मुँह से By Mouth IV नस में Intravenous IM मांसपेशी में Intramuscular SC त्वचा के नीचे Subcutaneous TAB गोली Tablet CAP कैप्सूल Capsule SYR सिरप Syrup INJ इंजेक्शन Injection UNG मलहम Ointment NEB नेबुलाइजर Nebulizer BP रक्तचाप Blood Pressure ECG हृदय की जांच Electrocardiogram CBC पूर्ण रक्त गणना Complete Blood Count डॉक्टर की लिखावट को समझने के लिए टिप्स फार्मासिस्ट से संपर्क करें: फार्मासिस्ट मेडिकल कोड और लिखावट जानते हैं। वे पर्चे को आसानी से समझेंगे। नियमित कोड सीखें: उपरोक्त चालिस कोड सबसे अधिक इस्तेमाल होते हैं, इसलिए इन्हें याद रखें। चिकित्सक से स्पष्ट करें: डॉक्टर से तुरंत पूछें अगर पर्चा समझना कठिन हो। डिजिटल पर्चे का इस्तेमाल करें: आजकल बहुत से डॉक्टर डिजिटल पर्चे देते हैं, जो सरल और स्पष्ट हैं। गूगल पर दवा का नाम खोजें: अगर आप दवा का नाम नहीं जानते तो ऑनलाइन खोज करें। You can read also:- Blood Sugar Level Chart: A Simple Guide to Normal Ranges निष्कर्ष शुरू में डॉक्टर का पर्चा समझना कठिन लग सकता है, लेकिन सामान्य कोड और उनके अर्थ जानने से यह आसान हो जाता है। इस ब्लॉग में दिए गए 20 कोड और टिप्स आपको डॉक्टरों की लिखावट और दवा के पर्चे को समझने में मदद करेंगे। यदि आपको कोई भी संदेह है, तो अपने चिकित्सक या फार्मासिस्ट से संपर्क करें। Related Blogs:
Brain Tumor: Types, Risk Factors, Symptoms, and Treatment
Introduction A tumor in the brain is one of the most serious and life-threatening conditions that can strike anyone, irrespective of age or background. Different types of brain tumors differ in cause and warning signs, which would help with early diagnosis and a better prognosis. Suspicious headaches, memory loss, or any brain tumor symptoms-there is something to look out for. This particular guide will go into the most common causes of brain tumors and who may be at high risk, with some treatment breakthroughs, as well as the medicines that are currently being used. From diagnosis through recovery, having the correct information makes a significant difference in dealing with this complex condition. What is a Brain Tumor? An abnormal increase in cells anywhere in or about the brain is termed a brain tumor. These tumors may be benign (non-cancerous) or malignant (cancerous), and their behavior depends on the kind, size, and location in the brain: they can grow slowly, causing no significant trouble for a long while, or act fast to block essential functionalities of the brain. Brain tumors either originate in the brain itself (primary brain tumor) or metastasize from some other parts of the body (secondary brain tumor). Depending on where they form, they can be problems facing movement, memory, vision, speech, or even personality. It is critical to recognize the early symptoms of brain tumors, like frequent headaches, problems with vision, or nausea of unknown origin, to have their diagnosis done early and undergo treatment. What Are the Early Symptoms of a Brain Tumor You Shouldn’t Ignore? Recognizing the first warning signs of a brain tumor might just save a patient’s life. At times, mild symptoms can be written off as an everyday problem—they are mistaken for stress or fatigue. Recognizing these symptoms of a brain tumor may aid in its early diagnosis and quick treatment. Here are some common early signs you should never ignore: Persistent headaches: A headache that either does not go away or increases in intensity over time, especially early in the morning or after the person lies down, can be one of the signs of a brain tumor. Visual or Auditory Changes: Patients with a brain tumor may experience blurred vision, double vision, or partial loss, depending on the location of the tumor. Other patients may complain of tinnitus or hearing loss. Memory Loss or Confusion: Difficulty concentrating, forgetting names or routines, or feeling mentally foggy can be signs of brain activity disruption caused by a tumor. Seizures: Any sudden seizure or convulsion appears in an adult who has never had one before. That is a serious signal pointing toward something affecting brain function abnormally. Balance Problems and Dizziness: Tumors located in the cerebellum or brainstem may impair coordination, balance, and physical movement. Nausea or Vomiting: Unexplained nausea and vomiting, especially in the morning, can be induced by increased pressure within the brain caused by a growing tumor. Changes in Personality or Behavior: A few rapid changes in mood or attitude could occur with a frontal lobe tumor: irritability and lack of motivation. You can read also:- Blood Clot in Brain: Types, Reasons & Treatment Why Do Brain Tumors Develop? Common Causes Explained Simply The causes of brain tumors can be quite confusing, mainly because even in most cases, there is no obvious reason behind their development. The medical sciences, however, with their knowledge concerning the factors possibly increasing the risk or directly causing the abnormal growth of cells in the brain, have managed to declare a few. As a way of taking care of your health or that of a dear one, it would benefit you to be informed of the potential causes of brain tumors so that you can keep a lookout and, if possible, take preventive measures.Here are some of the most common and scientifically linked causes of brain tumors: Genetic Mutations: Numerous brain tumors arise after some alteration, mutation, in the genes of some normal brain cells. The changes in DNA may cause the cells to divide without control into a mass of tissue called a tumor. Some of these gene changes may be inherited while others may arise during an individual’s lifetime. Family History and Genetic Conditions: Rare though it may be, a family history of brain tumors or some hereditary syndromes (such as Li-Fraumeni syndrome or neurofibromatosis) may predispose one to a brain tumor. Radiation Exposure: High doses of ionizing radiation, given either as therapy for cancer or owing to nuclear exposure, have been thought to increase the likelihood of developing brain tumors, especially in children. Age and Sex: Some brain tumors can develop at any age, while others are more common in children; still, more mature age is related to other tumor types, which, in turn, may be found more often in men and others in women. Weakened Immune System: People with immune system disorders, or those taking immunosuppressive medications, may be more likely to develop certain types of brain tumors, especially in the brain lining. How Is a Brain Tumor Treated? A brain tumor is treated based on many factors, such as its type, size, location, and whether the tumor is benign or malignant; with the patient’s age and general health, and specific symptoms of the brain tumor all playing a role in the development of the treatment program. In collaboration with the patient, once the diagnosis is established, doctors work to decide which treatment and action is most viable and safest for that individual. Here is a brief overview of the typical options for brain tumor treatment: Surgery: Should it be safe to perform, surgery is usually the first step. This means that they want to remove as much of the tumor as possible without incurring severe damage to the normal functioning brain tissue. A tumor can sometimes be completely removed, while occasionally only a partial removal is performed, followed by further treatment. The surgery also alleviates pressure from the tumor, leading to fewer headaches and seizures. Radiation Therapy: This method
Scalp Psoriasis: Symptoms, Causes, Treatment, and Further Insights

Introduction Scalp psoriasis is a long-term skin disorder that causes patches of red, itchy, and flaky skin on the scalp. If you’re constantly itching your scalp, flaking, or experiencing discomfort around your hairline, you might be having the symptoms of scalp psoriasis. It is important to know what exactly causes psoriasis on the scalp so that you can treat the scalp psoriasis properly and maintain your skin well. The symptoms, treatments for psoriasis, some diet tips for psoriasis, and the relation between skin inflammation and scalp issues are looked at in this guide. So, whether it’s something you have just been diagnosed with or something you’ve been suffering from for some time and want to learn more about treatment options, this article will be your guide to bring clarity and support. What is Scalp Psoriasis and Why Does It Happen? Scalp psoriasis is a chronic immune condition that affects the scalp, producing red, inflamed skin covered with silvery-white scales. It is one of the more frequent types of psoriasis, and the other symptoms usually include itching, flaking, and discomfort on the scalp. The particular scalp psoriasis symptoms may be mild to severe and can sometimes appear beyond the hairline onto the forehead, back of the neck, and behind the ears. Since scalp psoriasis is commonly mistaken for dandruff or some other scalp disorders, it always helps to have an idea of the early signs to seek proper care. The causes of scalp psoriasis are still unknown; however, it appears that it is probably the result of an overactive immune system that speeds up the process of skin cell regeneration. This abnormal cycling of skin causes dead skin cells to pile up and cause visible patches and skin inflammation. Triggers may include genetic predisposition, stress, climate change, and infections. Without an outright cure, that is a consolation: with the right scalp psoriasis treatment-from psoriasis medicine to topical application, a suitable psoriasis diet, the condition can be managed and kept in check. How to Identify the Common Symptoms of Scalp Psoriasis On noticing early symptoms of scalp psoriasis, prompt action can be taken toward healing and relief. If indeed persistent alterations are observed in terms of your scalp health, here are the most common signs to take note of: Persistent Scalp Itching – One of the early signs, an itchy scalp, is so irritating that it may affect one’s comfort level during the day and sleep at night. Red or Inflamed Patches – Areas of inflamed skin are usually raised patches of redness covered with thick, whitish, silvery scales. Flaking Like Dandruff – Unlike dandruff, these flakes accompany dry flakes with red skin underneath. Dry and Cracking – The scalp could feel tight and dry, which may crack and bleed in acute cases. Burning or Soreness – Some individuals feel burning or soreness along with itching of the scalp. Hair Loss – Though not a direct consequence of scalp psoriasis, harsh scratching or treatments do trigger a certain amount of temporary thinning or loss of hair. You Can Read also:- What is Ovarian Cancer? Causes, Symptoms, and Treatment Options What are the causes of Scalp Psoriasis? The understanding of psoriasis’ underlying causes is important in outbreak management and selection of appropriate treatment options for scalp psoriasis. Although the exact cause of scalp psoriasis is still unclear, it is often accepted to be an autoimmune condition where the body attacks some of the healthy skin cells. Below are some of the most common factors that might ignite or aggravate potential scalp psoriasis symptoms: Genetics – If someone in your family has psoriasis, you’re more likely to develop it too. An Immune System Overreaction – This causes your skin cells to regenerate too quickly, resulting in thick patches, skin inflammation, and scaling. Stress and Anxiety – High stress levels can trigger or even worsen scalp itching and other symptoms. Infections – Strep throat can induce the onset of scalp psoriasis in certain people. Certain Drugs – Medicines such as beta-blockers, antimalarials, and lithium have been associated with triggering psoriasis. Cold-Dry Weather – When temperatures drop, humidity levels follow, leaving the skin in want of moisture, a definite trigger for worsening symptoms of scalp psoriasis. Best Scalp Psoriasis Treatments That Work If flaking, itching, and redness of the scalp are bothering you because of scalp psoriasis, then the wonderful thing to remember is that you have several treatment options available. The right treatment for scalp psoriasis depends on the severity of your condition, but most patients do well with a mix of medical and lifestyle approaches. The treatments would mostly include: Medicated Shampoos and Topical Creams – They are typically the first line of treatment. They often contain salicylic acid, coal tar, and corticosteroids to reduce skin inflammation and scaling. Oral or Injectable Drugs for Psoriasis – Systemic therapy such as methotrexate, cyclosporine, or biologics targeting the immune response may be considered for moderate-to-severe cases. Phototherapy – UVB light therapy slows skin cell growth and reduces inflammation in the scalp. Scalp Oils and Moisturizers – Natural oils, such as coconut oil or aloe vera gel, help with dryness and itchiness of the scalp. Lifestyle Changes and Psoriasis Diet – Stress reduction, trigger avoidance, and following a psoriasis-friendly diet replete with anti-inflammatory foods can go a long way. How Does Diet Impact Psoriasis? Foods to Eat and Avoid While psoriasis, even scalp psoriasis, is immune system-driven, diet has much to do with how the human body reacts to inflammation and flare-ups. Eating a healthy, balanced psoriasis diet will keep you generally healthy and away from more skin inflammation, so your scalp psoriasis treatment will also work better on you. Some Helpful Food: The right food choices will keep the immune system calm and ease common manifestations of scalp psoriasis, such as itching, redness, and flaking of the scalp. Fatty Fish (Salmon, Mackerel, Sardines): High in omega-3 fatty acids that counter inflammation. Colorful Fruits and Vegetables: Loaded with antioxidants to help in skin repair and the general
Exploring the Normal Eye Pressure Range: What You Need to Know

Introduction Most of us visit the eye doctor for blurry vision, trouble reading, or the occasional headache. But there’s something your eye doctor checks that often flies under the radar—eye pressure. You may not feel it or notice it changing, but abnormal eye pressure can silently affect your eyesight and even lead to vision loss if left untreated. So, what exactly is the normal eye pressure range, and why does it matter? In this guide, we’ll walk you through everything you need to know—from how eye pressure works, to how it’s measured, what influences it, and when it’s time to seek medical attention. What is the Normal Eye Pressure Range? Your eye isn’t just a passive organ that captures images—it’s filled with fluids that keep it inflated and functioning properly. The pressure created by this internal fluid is called intraocular pressure (IOP), or more simply, eye pressure. The normal eye pressure range typically falls between 10 to 21 mmHg (millimeters of mercury). If your levels fall within this range, that’s usually a good sign that your eyes are healthy. But when eye pressure goes above 21 mmHg, it may indicate a risk for ocular hypertension, which could lead to glaucoma, a serious eye disease. Interestingly, not everyone with elevated pressure develops glaucoma, and some people can have glaucoma even with pressure within the normal range. That’s why regular checkups are so important—they help doctors see the full picture, not just a number. Why Maintaining Normal Eye Pressure Matters You might wonder—if I can’t feel it, is high eye pressure a big deal? The short answer: Yes. Eye pressure directly affects the optic nerve, the vital cable that sends visual signals from your eyes to your brain. When pressure gets too high, it can slowly damage the nerve over time. This damage is often painless and invisible until vision loss occurs—and at that point, it can’t be reversed. Maintaining normal eye pressure levels helps: Protect your optic nerve from long-term damage Reduce the risk of developing glaucoma Keep your vision sharp and clear Prevent future complications, especially as you age Think of it like blood pressure for your eyes. Just as you wouldn’t ignore high blood pressure, you shouldn’t ignore elevated eye pressure either. You Can Read also:- What is Ovarian Cancer? Causes, Symptoms, and Treatment Options Factors That Affect Eye Pressure So, what makes eye pressure rise or fall? Quite a few things. Some you can control—others, not so much. Here are some common factors: Age: Eye pressure can increase as you get older, which is why seniors are more at risk. Genetics: A family history of glaucoma or other eye conditions can make you more likely to develop high eye pressure. Medical conditions: Diabetes, hypertension, and thyroid disorders can all play a role. Medications: Steroid-based eye drops, creams, or pills can elevate IOP over time. Eye trauma or surgery: An injury or past eye surgery can interfere with the eye’s ability to drain fluid properly. Lifestyle: Lack of sleep, excessive caffeine, and smoking may also influence pressure levels. It’s also worth noting that your eye pressure isn’t static—it can fluctuate throughout the day. That’s why doctors often want to measure it more than once before making a diagnosis. How is Eye Pressure Measured? Checking your eye pressure is a routine part of a comprehensive eye exam. While it might sound a bit scary, the process is fast, painless, and completely safe. Here are a few common ways doctors measure it: Goldmann Applanation Tonometry This is the gold standard for measuring eye pressure. After numbing your eye with special drops, the doctor uses a tiny instrument to gently flatten a part of your cornea. It only takes a few seconds. Non-Contact Tonometry (The “Air Puff” Test) This is the one most people remember. A quick puff of air is directed at your eye, and the machine reads the pressure based on your eye’s resistance. It’s non-invasive and doesn’t require numbing drops. Tono-Pen and Rebound Tonometry These handheld tools are often used in emergency rooms or at-home settings. They’re helpful for people who may have trouble with the other methods, including young children or those with sensitive eyes. Each of these methods gives a reading of your current eye pressure and helps doctors determine whether your levels fall within the normal eye pressure range or require closer monitoring. When Should You Seek Medical Advice? One of the most challenging things about eye pressure is that you may not feel any symptoms until it’s too late. That’s why many people don’t know they have high pressure until they’ve already lost some vision. Still, there are signs you can watch out for: Symptoms of High Eye Pressure (or related issues): Blurred or hazy vision Eye pain or a heavy feeling in the eyes Halos around lights Headaches near the eyes or temples Sudden loss of vision (a medical emergency) Narrowing of peripheral vision over time If you’re experiencing any of these symptoms, it’s time to schedule an eye exam. Even if you’re symptom-free, regular visits to an eye specialist (optometrist or ophthalmologist) are essential, especially if you have risk factors like age, family history, or chronic illness. For those diagnosed with consistently high eye pressure or glaucoma, treatment might include eye drops, medications, laser treatments, or surgery. The good news? With early detection and proper care, vision loss from high eye pressure can often be prevented. You can read also:- Blood Sugar Level Chart: A Simple Guide to Normal Ranges Conclusion: Protect Your Vision by Staying Informed Your eye pressure might not be something you think about every day, but it should be on your radar. It plays a huge role in maintaining the health of your eyes and your ability to see clearly for years to come. Understanding and monitoring your normal eye pressure range isn’t just for those with eye problems—it’s a proactive step everyone should take. Whether you’re 25 or 65, taking a few minutes a year for an
Understanding Home Cholesterol Testing: Kits, Costs, and What Your Results Mean

Introduction Cholesterol levels directly affect heart health. Monitoring it will help reduce the chance of cardiovascular diseases, which rank among the top causes of fatalities in the world. The common method of checking cholesterol was to go into a clinic or hospital, draw blood, and have laboratory technicians work on it for several days. Modern technology development has now made it possible to check cholesterol at home. The popularity of home cholesterol kits is rising because of their convenience, privacy, and quick feedback. This article looks at everything you need to know about home cholesterol tests — how they operate, types of kits available, costs, instructions on using them, understanding results, and when to visit your doctor. Therefore, by the end of this article, you will know whether testing at home is for you and how to go about it. What Is Home Cholesterol Testing? Home cholesterol testing is what one would expect: a method to check one’s cholesterol levels without setting foot into a lab or hospital. These tests require a small blood sample customarily drawn from a fingertip prick, after which the results are either processed immediately by the testing kit at home or sent to a laboratory for analysis. The main purpose of these tests is to measure different types of cholesterol and fats present in your blood that have an impact on your heart health: Total cholesterol: The overall amount of cholesterol present in your bloodstream. LDL cholesterol (low-density lipoprotein): Considered “bad cholesterol” because its excess level causes clogging of arteries and increases the risk of heart diseases. HDL cholesterol (high-density lipoprotein): It is considered “good cholesterol” as it helps to clear bad cholesterol from your arteries. Triglycerides: A kind of fat in your blood-high levels may increase the risk of heart problems. Types of Home Cholesterol Test Kits An at-home cholesterol test kit is not a big category and comprises several types, trying to fit all conceivable purposes and budgets. Basic Cholesterol Test Kits: These are the simplest and cheapest kinds of cholesterol tests. Basic test kits normally test just total cholesterol. Essentially, they come with an included lancet-a tiny needle-for you to prick your own finger and test strips to which you apply the blood. After a minute or so, either the strip changes color, or a reading is shown on a tiny device. While these kits give you a quick snapshot, they don’t provide details on LDL, HDL, or triglycerides, which are important to know to get a bit more about your heart health. These kinds of cholesterol kits give you a fast snapshot but do not provide detailed information regarding LDL, HDL, and triglycerides, all of which are necessary for a more complete view of heart health. Full Lipid Panel Kits: More complete, a full lipid panel tests total cholesterol, LDL, HDL, and triglycerides. Depending on which way you want to go, these kits will use a digital reader for an instant display of results or ask you to send your blood to an outside lab, which then takes a few days to get back to you. This variety is suitable for those needing a larger look into their heart health, particularly if they have risk factors, e.g., family history, diabetes, or high blood pressure. Smart or Digital Cholesterol Test Kits: The newest of home testing technology, smart kits attach to your smartphone by Bluetooth or by a proprietary application. These kits provide a quick set of results and also keep the readings stored digitally, track trends through time, and can even share this data with your health provider directly. Smart kits are quite convenient and keep you aware of your health along the way, making them attractive options for tech-savvy users. You Can Read also:- What is Ovarian Cancer? Causes, Symptoms, and Treatment Options How Much Do Home Cholesterol Test Kits Cost? There is a wide range in prices in this home cholesterol testing kit market, depending on type and features: Basic kits cost somewhere between ₹500 and ₹1,000. Full lipid panel kits are charged anywhere around ₹1,500 to ₹3,000. In the case of smart kits, these can get pricier because of the added connectivity and app features they carry. How to Use a Home Cholesterol Test Kit Correctly The accuracy of the results depends greatly on the proper use of the kit. Here are stepwise guidelines: Read Instructions Carefully: No two kits are the same, meaning that you could not afford skipping reading the manuals. Following the best instructions will guarantee the best results. Prepare Your Body: Should fasting be necessary, do not eat or drink anything except water for 9-12 hours before the test to get the correct baseline reading. Clean Your Hands: Wash hands thoroughly before testing in warm water to increase blood flow and reduce contamination possibilities. Finger Prick: Prick the side of your fingertip using the lancet (it is less painful than the pad). Then squeeze it gently until the drop forms. Place Blood Sample on Strip: Cover the strip or cartridge fully, exactly following the instructions. Inadequate or excessive amounts of blood can throw the results off. Wait and Read Results: The appearance of the results takes only a few minutes; depending on the kit, they are either on a digital screen or characterized by a color change on the strip. Record Your Results: Keep a log of your cholesterol readings over time. This helps you and your doctor track any trends and make informed decisions. Understanding Normal Cholesterol Ranges Knowing what your cholesterol numbers mean is just as important in the test of knowing the test. The general guidelines for adults are as follows: Total cholesterol: Less than 200 mg/dL is considered desirable. LDL cholesterol (bad cholesterol): An optimal range is less than 100 mg/dL. HDL cholesterol (good cholesterol): A level of 60 mg/dL or above affords protection. Triglycerides: Less than 150 mg/dL is deemed normal. You can read also:- Blood Sugar Level Chart: A Simple Guide to Normal Ranges When Should
Why Is My Period Late? Signs and Symptoms

Book An Appointment Introduction An unexpected late period can be filled with confusion, worries, and curiosity, especially when one’s menstrual cycle is generally punctual. Pregnancy is most probably the first thought upon; yet, there are many other reasons for a late period that are nonspecific to pregnancy. Knowing the symptoms that arrive before a late period, and hormones linked with late periods, may help you find clarity on what is going on inside your system. In this article, we shall look into some of the common reasons for delayed periods, ways through which an irregular menstrual cycle may influence your health, and the early symptoms that one may spot even before a late period. We shall tackle such key factors and signs that challenge you through stress, lifestyle changes, and physical health concerns. Common Causes of Late Periods Late or missed periods are unsettling for women who follow a normal cycle. The stressful factors might bring alterations in the hormone profile of the woman, thus preventing a timely period. Therefore, knowing about such factors can help in identifying what could be going on and whether one should seek medical attention. Here are a few of the most common reasons for late periods in detail: Stress: High stress levels, emotional or physical, interfere with the hypothalamus, which is set to control your menstrual hormones. This imbalance, triggered by stress, can delay or even skip ovulation, resulting in a late period. Other symptoms before the actual late period may include tiredness, problems sleeping, and mood swings. The causes for delayed periods are related: 1.0. Hormonal Imbalance: Some common causes of late menstrual signs would be diseases like Polycystic Ovarian Syndrome (PCOS), hypothyroidism, or hyperthyroidism. Although PCOS causes higher androgen levels that interfere with the regular egg release, hypothyroidism or hyperthyroidism changes your menstrual cycle by altering your metabolism and hormone production. Weight Changes: Sudden loss of weight, obesity, or eating disorders can influence your body’s estrogen levels. When there is low body fat, there is a decrease in the production of hormones essential for ovulation, while excessive fat may cause excessive estrogen; either of these scenarios will cause menstrual irregularity or late menses. Excessive Exercise: Rigorous activities could affect hormonal alterations in menstruation, especially seen in athletes or in those who exercise without adequate caloric intake. The body enters an energy-saving mode, and it often results in missed or delayed menstruation. Illness: Acute illnesses such as flu and more chronic conditions such as diabetes and celiac may affect the menstrual cycle. Often, during an illness, the body can concentrate its energy on the functions deemed essential, and that could possibly perturb the hormone balance and cause late menses. Medication: Some medicines, such as antidepressants, chemotherapy, and hormonal contraceptives, could interfere with the menstrual cycle. For instance, going on birth control pills temporarily messes up our body’s natural hormone rhythm, causing irregular periods. Perimenopause: This is when women approach menopause, and hormone-level fluctuations occur. It heralds an irregularity of periods, with longer or shorter cycles, heavier or lighter flow, and sometimes skipped periods. Travel or Lifestyle Changes: Any sudden change in your daily schedule, such as flying across time zones or taking up night work, can dislocate the internal timetable of one’s body. These alterations can momentarily interfere with the hormonal signals that bring about the menstruation process. Pregnancy: Pregnancy is among the most common and frequent causes for late periods. In case your periods are late and you have had sex, taking a pregnancy test should be among your first thoughts. Other early signs of pregnancy may include breast tenderness, nausea, tiredness, and sporadic spotting. You Can Read also:- What is Ovarian Cancer? Causes, Symptoms, and Treatment Options Signs And Symptoms Of A Late Period As the missing or late period sets in, some early warning bodily signs can give you a clue that the menstrual cycle is out of sync. These signs will vary with the difficulty behind the late period, but mostly center around hormonal disturbances or interruption of the regular cycle of a woman’s body. A case of recognizing these signs may guide one to separate an occasional late period from an increasingly common situation of irregularity. These common symptoms may appear before the late period: Mild Cramping Without Bleeding: At the time your period is due, you might start to feel menstrual-like cramps, but then suddenly have no bleeding. This may indicate delayed ovulation or early pregnancy. Breast Tenderness or Swelling: Pre-menstrual or early pregnancy changes may make your breasts sore, heavy, or swollen. Fatigue or Low Energy: Feeling very tired may be connected to hormone fluctuations, stress, or pregnancy, which are all potential causes of late periods. Mood Swings or Irritability: Like PMS, mood swings can arise from hormone imbalance even when the time for your period is late or missed. Acne or Skin Changes: A sudden outbreak of oily skin could be a good hormonal signal for a late period, especially if you’ve got PCOS. Bloating or Changes in Digestion: Hormonal changes can sometimes cause bloating, flatulence, or irregular bowel habits. Symptomatic manifestation can erupt irrespective of whether your period is on time or delayed. Headaches or Migraines: Some people experience hormone-related headaches when the estrogen starts dropping in the premenstrual phase. A delay in the period may prolong or escalate the intensity of the symptoms. Change in Vaginal Discharge: An increase in vaginal discharge or a change in its texture (thicker or more slippery) can signal a late or imminent ovulation. Nausea and Food Sensitivities: Late periods due to pregnancy may be accompanied by nausea, heightened smell sensitivity, and peculiar food cravings or aversions. When to See a Doctor An occasional late period is usually nothing to be concerned about. But when such delays become a pattern or there is the presence of peculiar symptoms, they could point to a medical issue. It is imperative to consult a medical professional if your period comes late or goes for periods without arriving, and unusual symptoms